The healthcare industry continues to find itself in an entanglement with continuous risks.
Handling these risks implies the applicability of highly accurate predictive technologies that promise improved medical care.
Why does predictive modelling tools matter?
Were it viable sooner, the eminent 2020 Coronavirus global crisis would be manageable through quick and predictive algorithms. It would help contain the uprise of now prominent COVID-19 variants.
This article promotes predictive modeling in healthcare, its potential, implementation, and success factors.
Understanding predictive modeling
This statistical technique takes the approaches of data mining and machine learning technologies to forecast future data. In these approaches, historical and current data function as inputs.
On the other hand, future data is the anticipated output. Though this technique isn’t foolproof, it favors high accuracy rates.
How and where it can be used
Healthcare Routines
The healthcare industry primarily benefits from the outcomes of predictive modeling. Before thr predictive software development adoption, most healthcare resources catered to high-budget patients constituting a fraction of most patient databases. To chronic patients, this imbalance increases their readmission rates.
Surges Predictions
Health IT Analytics exemplifies the use of a predictive modeling approach to generate the COVID-19 index. The design and implementation of this predictive tool continue to be helpful to health agencies to anticipate and pinpoint potential COVID-19 pandemic surges.
Critical Patients Auto-detection
The predictability of this modeling approach does not stop here; it makes it easier to pinpoint prospective clients who fall under the category of critical healthcare patients.
Personalized and Affordable Healthcare
Also, using predictive modeling software as a healthcare tool delivers effective personalized patient care. It is easy to run patient pre-diagnoses and provide health remedies beforehand.
The predictability of this model benefits all the patients within a healthcare system. Also, its recorded analytics lowers healthcare costs and manages patients’ risks. The generated metadata from this model indicates the status and condition of all patients in the software system.
When their health status deteriorates, medical professions on duty get notified to take the needed preventive or curative steps. This patient is also safe from cumulative hospitalization bills.
Treatment Plans and Predictive Medicine
Predictive analytics consulting is key in providing an informed and organized healthcare service. The approach adheres to complex algorithms, spot-on procedures, and merited research patterns that lead to better treatment outcomes and uncovering new medical procedures.
Healthcare services and organizations cannot escape their future entanglement with this software modeling approach.
The Predictive Model’s Applicability
Its 2018 market value for developing predictive software was $2.904 billion. By 2026, its market value will project to an increased $22.4 billion. (Reports and Data).
Creating practical data is a major hurdle in this software modeling approach. Medics and healthcare providers need to envision valid healthcare approaches and fully execute the resulting insights.
It also requires creating a dedicated health management team that will follow up on high-risk patients and the immediate emergency contacts associated with them for on-time medical prescriptions and screening tests.
The developers of such healthcare software need to check certain boxes to create accurate healthcare models. Firstly, they need to define a problem statement before collecting the problem-related data (historical and current).
One aim of this modeling approach is to analyze input data accurately. For such a healthcare software model case, practical clinical data and accurate claims qualify as valid inputs.
The modeling process will take an approach similar to the following flow chart:
Predictive Modeling Process for Developing Healthcare Software
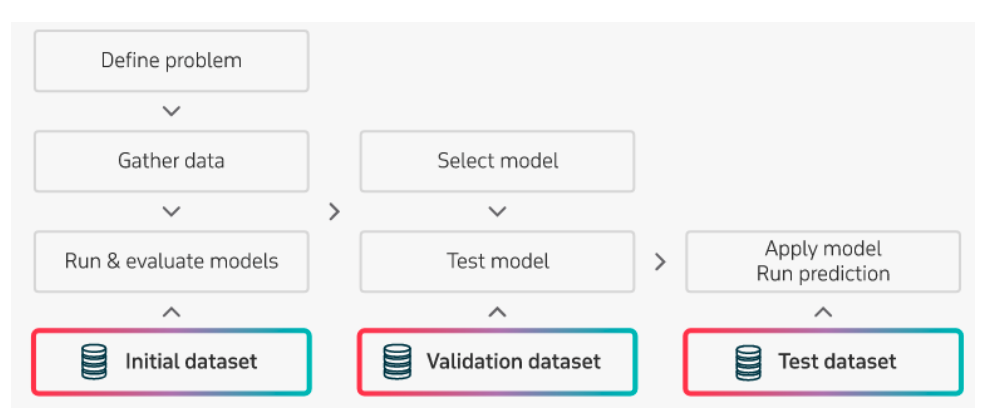
With several candidate models defined, an array of predictable variables helps produce effective and futuristic results. Executing some advanced tasks might be necessary. In this case, the model needs to implement neural networks for complex tasks or linear equations for simple tasks.
A defined problem is viable for a solution through data analyses and assessments of the various created models. The preferred modeling approach from these analyses and assessments is from the model that produces better results. It then becomes a simulation candidate for real-world or practical data.
Successfully integrated software models assist medical professions in dealing with potential patient risks leading to outcomes like:
- Avoiding patient readmissions
- Preventing suicide or patient self-harm cases
- Developing precise medical solutions and also determine its reactive effect on patients
Three factors determine this model’s success:
- Access Control: Continuous data processing and transmission mean that only authenticated and authorized users should be granted access privileges to patient data.
- Encryption: Patient data protection during wireless transmissions retains patient data integrity and reliability for future prognosis. Corrupt patient data can lead to a misdiagnosis.
- Data Storage: General Data Protection Regulations should govern data storage locations and how data processing should take place. Reliable data storage locations with viable regulations produce useful data.
Final Note
The use of predictive modeling to develop healthcare software is increasing slowly, steadily, and exponentially. The expansive use of wearable and remote care devices also pushes this agenda further.
The rapid adoption of predictive modeling in healthcare software faces security concerns and regulatory evolution as its main obstacles.
However, the advantages it offers in health operations overwhelm these fixable setbacks.

